By Douglas M. Wolfberg, Esq., EMT; and Stephen R. Wirth, Esq., EMT-P
On September 1, 2021, a Colorado grand jury handed down indictments in the case surrounding the death of 23-year-old Elijah McClain, who died after an interaction with police and EMS in Aurora, Colorado. The 24-page indictment charges two paramedics from Aurora Fire Rescue with 10 counts each of crimes including manslaughter, criminally negligent homicide, assault with a deadly weapon, conspiracy, and a range of other criminal charges. Three law enforcement officers were also charged with a variety of crimes.
It is extremely rare to see criminal charges brought against paramedics involving the care provided to a patient – and we are not aware of any case quite resembling this one. These are extremely serious charges in a high-profile case that will shine a national spotlight on many difficult and important issues regarding the delivery of EMS, the duties of EMS providers to their patients, the relationship of EMS and law enforcement and the role of medical protocols, specifically including those dealing with the use of ketamine.
The Presumption of Innocence is Critical
First, it is critical to remember that an indictment is a criminal complaint that is merely making allegations of illegal activity against the defendants. None of the allegations have yet been proven to be true in a court of law, and readers should not mistake a grand jury from a trial jury. A grand jury issues charges on behalf of the prosecution; a trial jury gets to decide if the allegations raised in the indictment have been proven. No such findings have yet been made in this case, and the defendants are presumed to be innocent of all charges.
Facts of the Case
The indictment sets forth certain “Essential Facts” underlying the criminal charges. Keep in mind that these facts are the prosecution’s version of the facts; their truth has not yet been established in court. Nevertheless, these are the facts as seen by the prosecutor as justifying the criminal charges, so we will review them as contained in the indictment documentation.
The incident occurred on August 24, 2019, when Mr. McClain, who was walking home from a convenience store, was approached by three Aurora police officers who had responded to a 911 call reporting a person who was wearing a ski mask and acting strangely. The officers concluded that Mr. McClain was “suspicious” and very shortly after engaging him, acted to physically “take control” of Mr. McClain. One officer told the other officers that Mr. McClain had reached for “your gun,” but the other officer stated that he did not feel any contact with his service weapon.
The police officers applied pressure to Mr. McClain’s carotid arteries in a technique known as a “carotid control hold.” Assorted other restraint techniques were also used by the police. The indictment also alleges that Mr. McClain vomited into his ski mask during the interactions with police but was unable to remove the mask or clear his own airway in his position of restraint. Mr. McClain lost consciousness at one point and the officers released the carotid control hold but at no time checked Mr. McClain’s pulse or breathing. At that time, the officers called for Aurora Fire Rescue to respond.
When the two paramedics from Aurora Fire Rescue (a non-transporting ALS first responder unit) arrived, they found Mr. McClain restrained and in handcuffs. Although the indictment alleges that the EMS crew was informed that a carotid control hold had been applied to Mr. McClain and that he previously lost consciousness, the two paramedic defendants deny having knowledge of the carotid maneuver. The indictment alleges that the two paramedics stood near Mr. McClain but did not speak to him or ask him questions.
The indictment alleges that the two defendant paramedics watched the police officers forcibly push Mr. McClain to the ground, and that one paramedic told the police, “we’ll just leave him there until the ambulance gets here and we’ll just put him down on the gurney.” After about two minutes on scene, the paramedics concluded that Mr. McClain was suffering from excited delirium. It is alleged that this determination was made by talking to the police officers and observing Mr. McClain for approximately one minute.
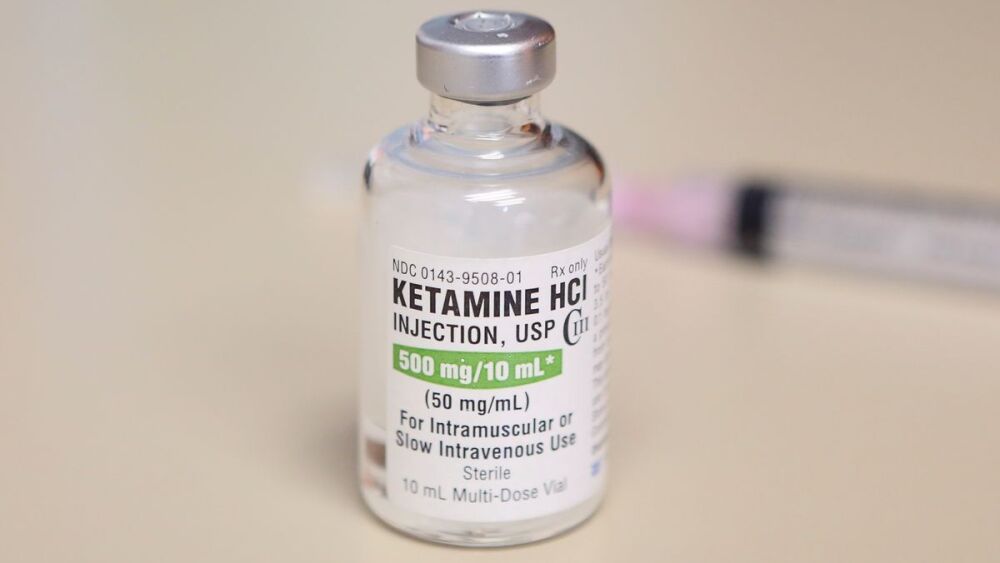
The indictment states that one of the paramedics ordered ketamine from the ambulance that had since arrived on the scene. The medic estimated Mr. McClain’s weight to be 200 pounds and dosed the ketamine at 500 mg. The indictment alleges that the correct dosage of 5 mg/kg would have produced a dose of 453 mg of ketamine if the medic had been correct in his estimation of Mr. McClain’s weight. In fact, the indictment alleges that Mr. McClain actually weighed 143 pounds, an overestimation of 57 pounds, and that the correct dose of ketamine should have been closer to 325 mg. About two minutes after the ketamine administration, Mr. McClain was placed on the ambulance gurney, unconscious and limp, with visible vomit on his face.
Shortly after loading Mr. McClain into the ambulance, the paramedics determined that he had no pulse or respirations and administered CPR and epinephrine. Mr. McClain regained a pulse but was declared brain dead three days later.
The Prosecution Theories Behind the Paramedics’ Charges
The charges against the paramedics include a total of ten criminal counts each. The theories underlying these charges are interesting and will break new legal ground if proven in court.
Based largely on the conclusions of an emergency room physician, the theories behind the charges against the paramedics center on a few important points.
- First, prosecutors allege that the determination of excited delirium “was an inaccurate diagnosis born of the paramedics’ failure to adequately assess Mr. McClain’s symptoms,” and in light of the “inaccurate diagnosis,” that ketamine should never have been administered.
- Second, the prosecutors allege that if ketamine administration had been appropriate, the correct dosage would have been 325 mg, not 500 mg.
- Third, the indictment states that the paramedics “deviated from the standard protocols governing when to administer ketamine such that the administration of ketamine was unlawful.” This allegedly unlawful protocol deviation resulted from:
- Improperly assessing Mr. McClain, leading to the alleged improper “diagnosis” of excited delirium;
- Failing to obtain a reasonable estimate of Mr. McClain’s body weight, leading to an administration of a dosage of ketamine that was too high (alleged to be an “anesthetic dose” of ketamine rather than an “subanesthetic dose”);
- Failing to properly monitor Mr. McClain during or after ketamine administration, causing Mr. McClain to suffer “multiple predictable complications”;
- Administering ketamine without obtaining Mr. McClain’s consent or even attempting to obtain his consent.
These theories raise critical legal issues that in some cases go to the heart of EMS patient care, operations, medical control and a host of other issues. Again, these factual allegations and charges are taken straight from the criminal indictment.
EMS Law Analysis
Our legal analysis and opinions are based solely on a careful and thorough read of the charging documents, in the context of our 25 years of practicing EMS law exclusively. We have not reviewed the clinical documentation nor have we been consulted in this case, or spoken to any parties involved.
Based on the theories advanced by the prosecution, the overriding issue in this case legally appears to be the attempt to “criminalize” acts of medical malpractice and to make deviation from EMS protocols a crime. Of course, we are not saying that there was medical malpractice or protocol deviation; those are facts which have not yet been proven in court. We are now simply analyzing the indictment and the prosecutors’ theories.
First, even if it is true that the paramedics in this case failed to make an incorrect determination of excited delirium, it will be a high hurdle for the prosecution to prove that such a failure rose to the level of intent or culpability – or even criminal negligence – required in a criminal case. Intent – or the “guilty mind” – is basically a continuum under the law. There are three general categories:
- Negligence. Basic medical malpractice is a form of negligence, which is an unintentional act.
- Gross Negligence. In most states, to win a malpractice case against EMS providers, the plaintiff must prove gross negligence, which is something more than ordinary negligence. It typically requires evidence of extreme indifference or reckless disregard for the health or safety of others.
- Both negligence and gross negligence – which are civil matters as opposed to criminal cases – require only proof by a “preponderance of the evidence,” that is, the scales need only tip ever so slightly against the defendants for the plaintiff to prevail.
- Intent. Finally, intent is at the top end of the continuum; it requires proof that the defendant willfully and purposefully committed an act in violation of the law. This is the most difficult standard of proof, and instead of proof by a preponderance of the evidence, conviction in a criminal matter requires proof “beyond a reasonable doubt,” which is a more exacting legal standard making it much harder to prove in court than negligence or gross negligence.
The types of allegations made by prosecutors in the McClain indictment are those ordinarily seen in civil medical malpractice cases. The prosecution here has its work cut out for it, because it essentially needs to show that the paramedics willfully and purposefully – or with criminal negligence – “misdiagnosed” Mr. McClain and then overestimated his body weight in order to then justify the improper administration of Ketamine at an impermissibly high dose.
First, this will require the prosecution to deal with what a defense expert will almost surely point out as a prosecutorial overreach: that is, the traditional view that “diagnosis” is not within the EMS scope of practice. Second, even if the paramedics made the wrong call in concluding that Mr. McClain suffered from excited delirium, it will be very difficult for the prosecution to prove that they did this with malicious criminal intent, i.e., a “guilty mind,” or even criminal negligence.
The prosecution here is also trying to break new ground in essentially “criminalizing” EMS clinical protocols. The theory underlying these charges is that the violation of the clinical protocols on ketamine administration made the paramedics’ actions unlawful. Protocol deviations are certainly quality of care issues, and their violation has been the basis for countless civil suits alleging medical malpractice. But the prosecution theories in the McClain case essentially turn protocols – medical procedures that may vary considerably from one community to the next – into statutes or regulations. That is simply another potential overreach with little precedent that will be interesting to see play out in a court of law, if this case goes to trial against the paramedics.
This is not to say that actions of an EMS provider in violation of clinical protocols could never rise to the level of criminal conduct. For instance, if a protocol says to “administer oxygen” and the provider chooses to administer it by hitting the patient in the head with a D-cylinder, that particular protocol deviation surely constitutes a criminal assault. But to base charges of criminal assault and manslaughter on an allegedly improper patient assessment, allegedly incorrect “diagnosis,” and an allegedly improperly estimate of patient weight is to transform what are ordinarily negligence principles into crimes. This will be the groundbreaking challenge facing the prosecution team, and if this case goes to trial, it will be done under the intense glare of a national media spotlight.
Broader Lessons and Cautionary Tales
Regardless of whether the prosecution against the two Colorado paramedics results in a dismissal, an acquittal, a conviction or a plea bargain, the McClain case brings into specific focus some broader issues for EMS agencies nationwide to consider and reflect upon. Please note that in this section of the article, we are not referring to the McClain case or any other specific case; these are merely general thoughts prompted by some of the recent nationally publicized cases against law enforcement alleging excessive force and civil rights violations.
EMS and the police in many communities have a close and positive working relationship. They often rely upon each other and work together at the same scenes. In many places in America, police officers and EMS personnel work for the same employer, typically a municipality or county. The public almost always benefits from this close collaboration.
However, there are times when the relationship between law enforcement and EMS can be harmful to patients and put EMS providers in a bad spot.
In some cases, particularly involving combative, armed, violent or mentally ill patients, the goals of law enforcement and EMS may be fundamentally incompatible. Law enforcement may seek to subdue, restrain, neutralize and control a suspect, sometimes with techniques, devices and weapons that even when authorized and properly used can be dangerous. EMS providers, on the other hand, are not agents or tools or adjuncts of law enforcement. EMS providers do not exist to assist police officers in their tasks of subduing or restraining patients. EMS providers have a duty of care to a patient. They must act as patient advocates, regardless of how exactly that person came to be a patient, and regardless of that person’s ethnic background, economic status, station in life, or neighborhood where they may be found. In other words, EMS works for the patient, not law enforcement.
For example, if law enforcement is actively subduing a suspect and asks for EMS to administer a drug to assist in that process, that alone would be an improper reason to administer that drug. If, however, after a proper patient assessment, the EMS provider determines that the use of the drug is clinically appropriate, based on applicable online or off-line medical control such as protocols or standing orders, then the use of the drug would be appropriate regardless of the fact that law enforcement requested it. The point is that EMS providers must base their patient care decisions only on clinical considerations, and not for the sole reason of assisting law enforcement with their tasks.
Another example: say for instance that the police have restrained someone in a prone position with handcuffs behind their back. EMS arrives and is told by the police to “take this sonofabitch to the hospital but keep him face down and his hands cuffed behind his back.” Regardless of whether the police had a proper and lawful reason to restrain the person in this manner, the EMS crew cannot simply comply with the direction of the police and do nothing more. They must assess and continually reassess the patient, and if the patient is found to require circulatory or ventilatory support, or other necessary treatment, they must reposition the patient and provide the care regardless of the instructions given by the police to “keep him face down.”
These scenarios may certainly give rise to claims of medical malpractice or negligence, but as the McClain case shows us, they can also lead to criminal charges. In addition, where the EMS providers are employees of a public sector agency, such as a municipal fire department or third service EMS agency, they can also find themselves as defendants in civil rights cases. For instance, if it is alleged that law enforcement wrongfully used force in violation of an individual’s civil rights, and EMS simply showed up and complied with the orders of law enforcement, or silently cooperated with them without conducting an adequate assessment or providing proper patient care the EMS practitioners may find themselves in the courtroom right next to the police officers under the glare of a nationally televised trial.
Conclusion
The indictments of the paramedics who were called to treat Elijah McClain will be closely watched and may change expectations and practices for EMS. The prosecution of these paramedics seeks to break new legal ground, and if the prosecutions are successful, may rewrite the rules in cases where EMS and law enforcement interact. But regardless of the outcome in this case, EMS providers should take lessons raised by this and other cases as a cautionary tale in remaining patient advocates in high-pressure law enforcement situations.
Read more
Patients in custody and in need of treatment
Every EMS provider and leader has an obligation to heed the important lessons from the Elijah McClain case. Doug Wolfberg and Steve Wirth have written eight recommendations for EMS providers and leaders.